Lambert-Eaton Syndrome
What is Lambert-Eaton syndrome?
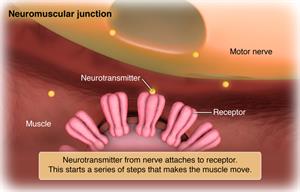
Lambert-Eaton syndrome is also known as Lambert-Eaton myasthenic syndrome. It is a rare, autoimmune disorder in which the immune system attacks the neuromuscular junctions. These are the areas where your nerves and muscles connect. Normally, your nerve cells pass signals along to your muscle cells. These signals help your muscles move. Lambert-Eaton syndrome affects the way your nerves and muscles communicate, making it hard to move your muscles as you normally would.
What causes Lambert-Eaton syndrome?
This condition is often associated with a certain type of cancer called small cell lung cancer. This syndrome may result from your body's efforts to fight the underlying cancer.
In some cases, Lambert-Eaton syndrome develops following another autoimmune disease. Sometimes the cause is not known.
What are the symptoms of Lambert-Eaton syndrome?
These are possible symptoms of Lambert-Eaton syndrome:
-
Weak muscles (weakness is often relieved for a short time after exercise or exertion)
-
Trouble walking, climbing stairs or getting up from a chair
-
Tingling sensation in the hands or feet
-
Eyelid drooping
-
Fatigue
-
Dry mouth or dry eyes
-
Trouble speaking and swallowing
-
Trouble breathing
-
Bladder and bowel changes
-
Erectile dysfunction
-
Decreased sweating
-
Weight loss
How is Lambert-Eaton syndrome diagnosed?
Your healthcare provider will review your symptoms with you and do a physical exam. A special antibody blood test may show that you have this condition. You may also undergo a test called electromyography, which shows how well your muscles are working. Because Lambert-Eaton syndrome is associated with lung cancer, your provider may order X-rays or a CT scan of your lungs. Another condition called myasthenia gravis has symptoms that are very similar to Lambert-Eaton syndrome. Your healthcare provider will use the results of the electromyography and other tests to tell the difference between the conditions.
If your healthcare provider finds that you have this condition, you'll be checked for lung cancer and other cancers, such as lymphoma. If cancer isn’t found at first, you may need regular screenings or CT scans for up to 5 years checkups to keep looking to watch for an underlying cancer. That's because Lambert-Eaton syndrome may appear as much as 3 years before a cancer diagnosis.
How is Lambert-Eaton syndrome treated?
If you have cancer, your healthcare provider may treat it with surgery, radiation, or chemotherapy. If you have cancer and respond well to treatment, your Lambert-Eaton syndrome is more likely to get better. Your provider may also prescribe medicines to suppress your immune system or to help improve the signals between your nerve and muscle cells.
You may also undergo a treatment called plasmapheresis. This involves replacing the plasma in your blood. This removes harmful immune system proteins from your blood that may be involved in the condition.
What can I do to prevent Lambert-Eaton syndrome?
Because the exact cause of Lambert-Eaton syndrome isn’t fully understood, it’s not entirely clear how to prevent the disease. The best way to reduce your risk for lung cancer, often associated with Lambert-Eaton syndrome, is not to smoke. Other steps that may help lower your risk for lung cancer include:
-
Staying away from tobacco smoke
-
Eating more fruits and vegetables
-
Having your home tested for elevated levels of radon gas
-
Reduce exposure at the workplace to cancer causing substances, such as asbestos, arsenic, nickel, and chromium
Living with Lambert-Eaton syndrome
Symptoms of Lambert-Eaton Syndrome may become worse when you're warm or have a fever. As a result, don't take hot showers or baths. Contact your healthcare provider if you start developing signs of a cold or the flu. Exercising on a regular basis and getting enough sleep may also help you manage your symptoms.
Key points about Lambert-Eaton syndrome
-
Lambert-Eaton syndrome is a rare, autoimmune disorder in which the body's immune system attacks the connections between nerves and muscles. It is most often seen in people with small cell lung cancer or other cancers, but it can also occur in people without cancer.
-
Common symptoms are weak muscles, trouble walking, tingling sensations, fatigue, and dry mouth.
-
If there is an underlying cancer, finding and treating it is the first priority. That may improve symptoms from this condition. Other treatments include medicines to suppress the immune system or to help make the signals stronger between the nerves and muscles.
Next steps
Tips to help you get the most from a visit to your healthcare provider:
-
Know the reason for your visit and what you want to happen.
-
Before your visit, write down questions you want answered.
-
Bring someone with you to help you ask questions and remember what your provider tells you.
-
At the visit, write down the name of a new diagnosis and any new medicines, treatments, or tests. Also write down any new instructions your provider gives you.
-
Know why a new medicine or treatment is prescribed and how it will help you. Also know what the side effects are and when they should be reported.
-
Ask if your condition can be treated in other ways.
-
Know why a test or procedure is recommended and what the results could mean.
-
Know what to expect if you do not take the medicine or have the test or procedure.
-
If you have a follow-up appointment, write down the date, time, and purpose for that visit.
-
Know how you can contact your healthcare provider if you have questions, especially after office hours or on weekends.